Through the years and the development of pharmacology, Antimicrobial resistance (AMR) is a growing public health threat of broad concern to countries. Recently, the World Health Organization (WHO) produced a global report on surveillance of antimicrobial resistance in collaboration with Member States. This report monitors the situation worldwide, showing that the percentage of antibiotic resistance to various diseases is growing year after year all over the world, especially in developed countries, and the resistance to common bacteria has reached alarming levels in many parts of the world. It indicates that many of the available treatment options for common infections in some settings are becoming ineffective.
According to those who prepared the report, “a post-antibiotic era—in which common infections and minor injuries can kill—far from being an apocalyptic fantasy, is instead a very real possibility for the 21st century.”
Particularly, the report focuses on antibacterial resistance (ABR), which involves bacteria that causes many common infections for which treatment is becoming difficult. The main focus of this report is therefore on ABR for which knowledge, support and concerted action are inadequate. The report considers seven types of antibacterial resistance pathologies and their respective drug treatments:
- Escherichia Coli vs. the third-generation Cephalosporins and vs. Fluoroquinolones
- Kleibsiella Pneumoniae vs. the third-generation Cephalosporins and vs. Carbapenems
- Staphylococcus Aureus vs. Methiccilin
- Strptococcus Pneumoniae vs. Penicillin
- Non Typhoidal Salmonella vs. Fluoroquinolones
- Shigella Species vs. Fluoroquinolones
- Neisseria Gonorrhoeae vs. 3rd generation Cephalosporins
The first important finding of the report is that there are many gaps in information on pathogens of major public health importance. In other words, the information gathered highlight the strengths and weaknesses in both the collection of data collected in Member States and their quality, and it seems to demonstrate that a global consensus on methodology and data collection for ABR surveillance is still missing. For instance, data on E. coli resistance to third-generation cephalosporins were obtained from only 86 (44%) of the Member States, while those on the resistance to fluoroquinolones from 47% of the Member States. About Kleibsiella Pneumoniae, data on carbapenem resistance from 71 (37%) of the countries, and, concerning Neisseria Gonorrhoeae, data were obtained only from the 22% of the Member States. Furthermore, data were collected in a non-homogeneous way, which makes it difficult to make comparisons or draw maps. Finally, all the national reports refer to different periods: a single year or a longer period. Nevertheless, it is possible to outline a main trend. Even if the European Region has a good percentage of reporting data (79%) the region with most of the countries that have provided the information is the South-East Asia Region (82%).
South-East Asia Region
Up to 2011, data reveal that in this area the antibacterial resistance was a burgeoning and often neglected problem. However, three years ago the health ministers of the region’s Member States articulated their commitment to combat AMR through the Jaipur Declaration on AMR. Since that moment, all the 11 Member States have decided to contribute information for a regional database and they agreed to participate in a regional consultative process.
Western Pacific Region
70 percent of the Western Pacific Region provided information concerning ABR. Actually the situation is not uniform: even if in some of the high-income countries there is a long established system for routine surveillance of ABR, there are still gaps in geographic coverage and a lack of surveillance in community settings. In this sense, some Pacific Island suffer the consequences of being isolated and to the lack of human resources.
American Region
The enormous variety of the American continent makes the American Region a very complex area to analyze. Since 1996, the WHO Regional Office for the Americas/Pan American Health Organization (AMRO/PAHO) led ReLAVRA, the Latin American Antimicrobial Resistance Surveillance Network, with the aim of collecting aggregated data provided by national reference laboratories. Moreover, in Latin America is still active, since 1993, the Sistema de Redes de Vigilancia de los Agentes Responsables de Neumonias y Meningitis Bacterianas, called SIREVA II, initiated by AMRO/PAHO to provide a regional monitoring programme for important bacteria causing pneumonia and meningitis.
African Region
Concerning the African Region, the surveillance of drug resistance is carried out in only a few countries and there is not awareness of the consequences of infectious conditions for public health. However, even if we have just few groups of information, available data indicate that the African Region shares the worldwide trend of increasing drug resistance, particularly for several bacteria that are likely to be transmissible not only in hospitals but also in the community.
East Mediterranean Region
Data reveal that the East-Mediterranean Region must achieve several challenges, as the absence of legislation and the disruption of basic health services. However, reports and studies from some countries in the region show the geographically extensive emergence of ABR, especially due to the collection of resistance information from disease-specific programmes, for example TB, HIV and malaria. Finally, concerning the European Region, the following map, based on WHO dataset, shows the situation concerning each Member State. Due to the lack of uniformity in collecting data, the graph shows only data collected in 2011, only in this way we could compare the situation among different countries.
Another equally important aspect concerns the surveillance of antimicrobial drug resistance in disease specific programmes, especially on TB and HIV programmes. The following map is very clear: the majority of the country worldwide notified at least one case of extensively drug-resistant TB (XDR-TB) by the end of 2012, in particular, it was estimated that during the same year, on a global level, 20.2% of previously treated cases had multidrug-resistant TB (MDR-TB), especially in Eastern Europe and central Asia.
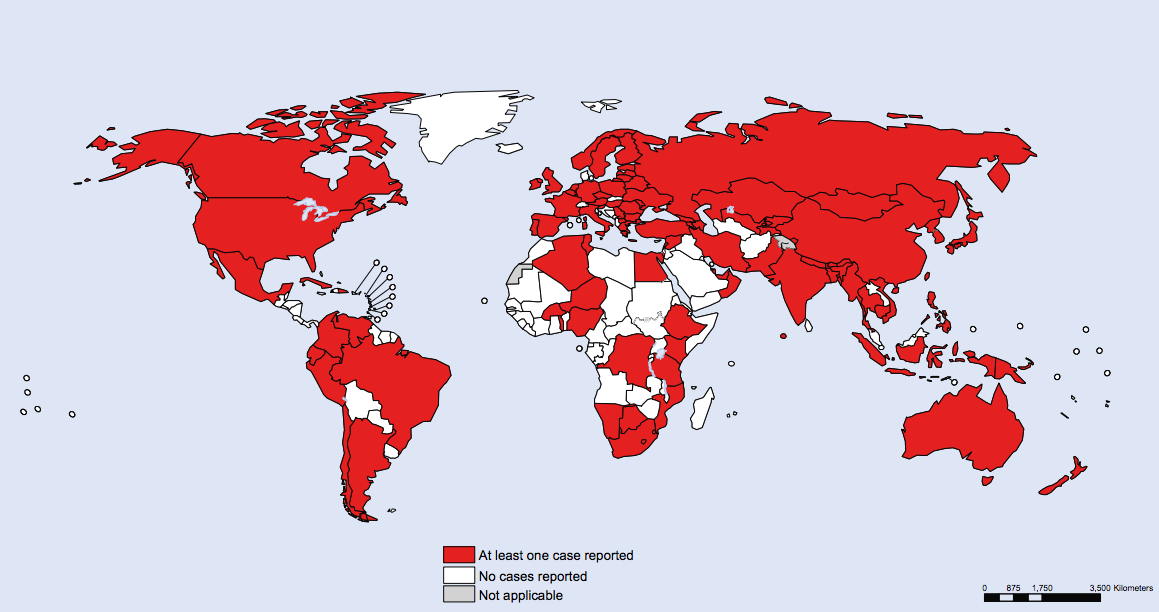
Even in European Region, the situation seems to be dangerous: we have the highest percentage in the world of multidrug-resistant cases both among new and previously treated TB patients, due to the fact that in affluent countries the percentage of drug treatment is certainly greater than the rest of the countries.
Concerning HIV the multidrug-resistance has enormous consequences on HIV treatments like Antiretroviral therapy (ART) that slow down the progression of the disease by preventing the virus from replicating and thus decreasing the amount of virus. HIV drug resistance causes ART failure, so minimizing the emergence of HIV drug resistance and its transmission is critical to ensure the continued effectiveness of Antiretroviral therapy.